Teamwork, planning key to NIHD’s coronavirus response
- Category: NIHD News
- Posted On:
 It is an overused analogy, the war against novel coronavirus, but as any employee at Northern Inyo Healthcare District will tell you, the battle is real. Ironically, it is a battle most have prepared for throughout their respective careers.
It is an overused analogy, the war against novel coronavirus, but as any employee at Northern Inyo Healthcare District will tell you, the battle is real. Ironically, it is a battle most have prepared for throughout their respective careers.
“Every team member brings something to the fight,” says Dr. Stacey Brown, Medical Director of NIHD’s Rural Health Clinic and current Vice Chief of Staff. “Every department plays a role.”
For NIHD Board President Jean Turner, the show of teamwork fits right into the District’s operational design. “When I came onto the Board, I was told our basic structure is that of an inverted pyramid,” Turner says. “Leadership at the bottom, the workforce at the top. The top is where the real work goes on; it’s where things really matter. If I wanted our community to remember one thing at this point in time, it’s this: Our staff is disciplined, well-trained, and ready for this challenge.”
The District’s fight against coronavirus began in mid-January. For weeks, Infection Preventionist Robin Christensen, RN BSN HIC, kept an eye on what was transpiring in China. On January 28, she called the first team meeting to talk about coronavirus and its potential impact on NIHD and the community. Everyone in the room knew the odds, had watched the numbers coming in from China.
“It is safe to say we wished for the best, but as healthcare workers, we always prepare for the worst,” Christensen says. “It’s who we are; it’s what we do; it is what the community expects from us at a time like this.”
As the NIHD team developed needed plans, they carried on with providing day-to-day care. Hallway conversations and internal emails began to refer to coronavirus more frequently. The District conducted a pandemic disaster drill on February 13. The tipping point came March 6 when a two-hour coronavirus meeting gave way to a day-long review of staffing levels, supplies, policies, plans, and shared concerns.
The group met the next afternoon again for several hours. They got a late start, beginning at noon. It gave those who volunteered to help at the Eastern Sierra Cancer Alliance’s Blue Ribbon Walk & Run a chance to meet their commitment. For many at NIHD, it was the last “normal” day of the month.
NIHD initiated an internal Incident Command on March 10 and continues working under it today. Incident Commands use a standardized approach to direct, control, and coordinate emergency response. More importantly, it brings people together to reach a common goal.
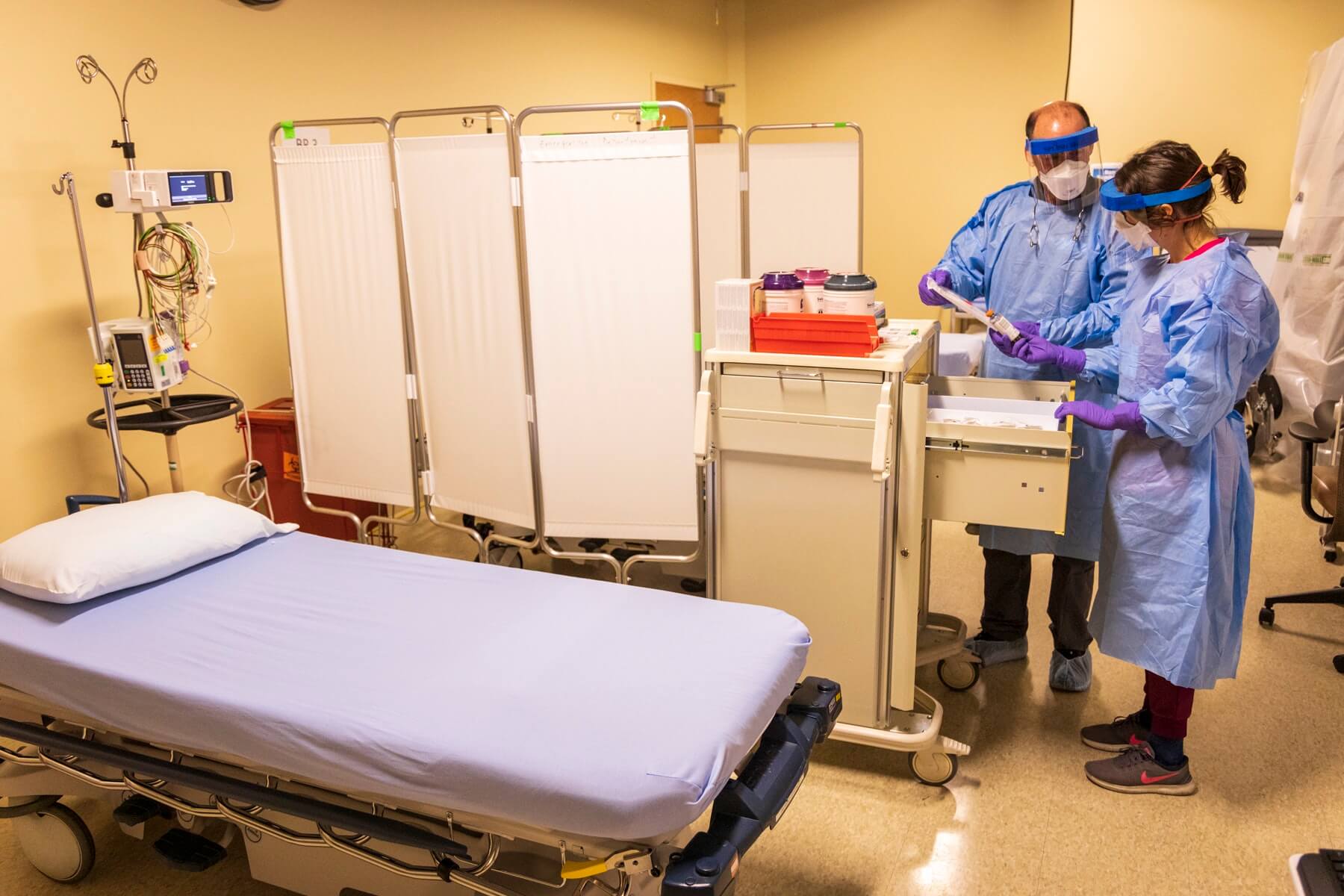
Like her co-workers, this was not the first time Allison Partridge, RN MSN, worked under an Incident Command. Partridge, the Director of Nursing for the Emergency and Medical-Surgical departments, knows the system well and aids Chief Nursing Officer Tracy Aspel in keeping the daily meetings on task.
Partridge now spends much of her days working with others to put together workflows for the departments that will be most affected. With guidance from Infection Preventionist Christensen, Partridge and others closely watch the Centers for Disease Control and Prevention and the California Public Health Department for direction. No area or service escaped review.
“We track daily our current availability of Personal Protective Equipment (PPE), and the recommendations for use,” Partridge says. “Additionally, we have made modifications in how we provide services and how visitors access the campus. All of these measures are in place to protect our teams and community. We encourage all employees to adhere both while at work and at home to the recommendations issued by national, state, and local government.”
Carefully crafted plans address the care of Patients Under Investigation (PUIs). Partridge says the standardized workflows are based on the patient’s level of care, whether that be critical care at the hospital or self-isolation at home. Care of multiple positive COVID-19 patients within the hospital remains an area of concern for the small 25-bed hospital.
“A great amount of planning and preparation has gone into every action, and it’s still ongoing,” Partridge says. She notes that just this week, the team was searching every square inch of the facility for places to place more beds. No space is overlooked. An unused and unfinished room located in the two-story hospital was turned into a four-bed safe patient care area within hours.
As for staffing, the level is adequate at this time. The District is working closely with the American Federation of State, County, and Municipal Employees Union on staffing plans should the virus take hold of the community.
As non-essential services are scaled back, staff in those areas become available for use in others. Nurses and caregivers were surveyed to see if they would be OK to serve in other departments they were cross-trained to work in. Recently retired nurses may be considered for voluntary return to bolster staffing numbers. The dedicated care given by generations of NIHD nurses is legendary in the community.
They were also asked who would be willing to work with critical coronavirus cases. No one will be asked to step into a situation they are uncomfortable with -- and to date, no one has opted out.

As for the physicians, Dr. Brown and Dr. William Timbers, NIHD’s Chief of Staff, are relying on the aid and advice of many of the District’s Medical Chiefs – Dr. Richard Meredick (Orthopedics), Dr. Charlotte Helvie (Pediatrics), Dr. Sierra Bourne (Emergency), and others. The Medical Support Staff office issued emergency credentials for other physicians in the area should their aid be required at bedsides.
The Rural Health Clinic team launched drive-in coronavirus testing well before some larger, urban hospitals did. The move was based on when the RHC offered drive-in flu shots more than a decade ago. “Hometown health care can work anywhere, even in the big city,” Dr. Brown smiles.
Dr. Brown’s reliance on RHC Directors Paul Connolly and Jannalyn Lawrence, RN, is evident. Both work closely with the District’s outpatient clinics and played critical roles in clearing barriers for drive-in testing. When offered kudos for the work, Lawrence scoffed. “One Team, One Goal,” she says, incurring the closing line of the District’s mission statement.
Later, as Director of Nursing Partridge studies the endless worklists that paper the walls of Incident Command, she agreed with Lawrence. “Teamwork has played a huge role in managing every aspect of this situation,” she says. “This collaboration has taken place across all disciplines and has included a multiagency approach across Inyo and Mono counties. This great work truly exemplifies our mission of ‘One Team, One Goal, Your Health.’”
Meanwhile, as another day ends for the District team, Infection Preventionist Christensen is in her office. It is quiet in the usually bustling hallway; the result of the District’s temporary telework plan. Almost 80 employees are working from home, practicing social distancing.
Laying across Christensen’s desk are signs of a community lending its support to its healthcare workers: Packages of the valued N95 masks recovered from businesses and home garages, plus several handcrafted face masks. The handcrafted masks, with bright patterns of cacti, cats, and paisley, are especially touching to Christensen.
NIHD is looking into options that could allow the homemade masks to be used as covers for approved personal protective equipment. That would occur if, and only if, NIHD’s supply of approved masks is depleted. The covers would help keep the N95 masks free of transferred hand oils, possibly extending the life of the N95s.
“One team,” Christensen says, circling her index finger, gesturing from east to west, north to south. “It’s all of us in the community. Together, we will get through this.”


